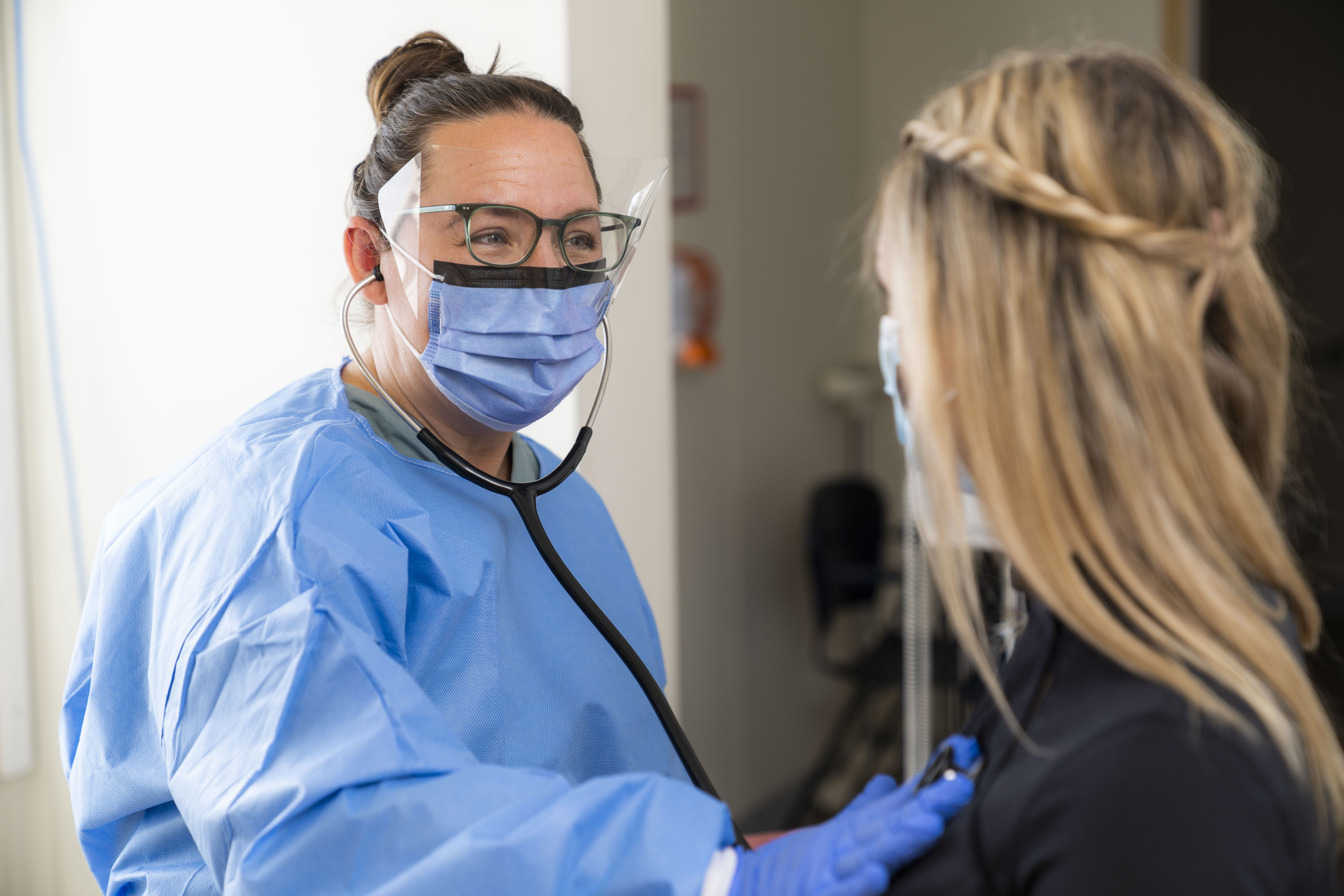
Throughout the COVID-19 pandemic, the word “virtual” has become a common part of our vocabulary. In order to stay safe, people attend Zoom business meetings, worship services, concerts and events; they meet virtually with loved ones over apps like FaceTime; and they take courses, receive tutoring and access counselling services, all by phone or video conferencing. However, as convenient as virtual meetings can be, many health-care services must be delivered in person. This includes some of the care provided by Dr. Kelsey Kozoriz.
Dr. Kozoriz helms the Cowichan District Hospital (CDH) Respiratory Assessment Clinic, one of several clinics developed across Island Health to allow primary care providers, in response to the need to limit in-person community office visits during the COVID-19 pandemic, to refer people with mild respiratory symptoms to be seen in person. What makes the CDH clinic unique to Island Health is for the last several months the clinic has expanded its scope to also provide virtual and in-person care to those who do not have a primary care provider.
“It’s been so rewarding to support people who don’t have a family doctor through an acute illness, helping to reassure them through their fears and worries, including some of the stigma associated with COVID-19, and connecting them with resources they might not know about, like intensive home health monitoring,” says Dr. Kozoriz. “However, it’s not just me working independently. I’m part of a bigger system, including public health and community health services, working together to provide care to our patients.”
The service is called the Cowichan Valley Virtual COVID Ward, and since January, nearly 100 people with COVID-19 have received care from Dr. Kozoriz. Given that Dr. Kozoriz is also responsible for Cowichan’s COVID-19 testing centre, she gets in touch swiftly with patients who have received a positive result to provide advice and care that includes referrals to mental health services and at times, support with food and medicine for those who are isolating.
“At the beginning of 2021, COVID cases in the Cowichan region rose significantly and that’s when we started to notice a gap in care for people who didn’t have a family doctor to call for advice. There was also concern that some patients were going to hospital late in their COVID-19 illnesses – we needed a way to ensure those who were unattached that they could be supported by a physician alongside our public health teams,” she says. “And, if their symptoms worsened, we could examine them in person, which offered comfort and reassurance.”
Dr. Kozoriz also developed key relationships, such as with Island Health’s Intensive Home Health Monitoring Program, which allows her to monitor a patient’s oxygen levels while they are isolating. In addition, she reached out to Cowichan Primary Care Network (PCN) staff and Dr. Troy McLeod at Slhexun Sun’ts’a Primary Care Clinic to explore the possibility of connecting the unattached COVID-19 patients to a primary care provider. Through conversations with these clinics, patients with COVID who had completed their isolation period were identified as a priority population to attach. As such, Dr Kozoriz, the PCN, and Slhexun Sun’ts’a successfully facilitated referrals of 17 people to a primary care provider in the Cowichan Valley.
“If any of those patients end up having long COVID or persistent symptoms, we want to ensure they are attached and well cared for after their infectious period is over,” she says. “The process has been started for anyone who has asked to be referred for attachment.”
Early in 2020, Dr. Kozoriz set up a similar virtual clinic that ran for several months with the support of partners including the Cowichan Valley Division of Family Practice, with COVID project funding support from the Cowichan District Medical Society. That clinic was aimed at helping patients navigate the frequently changing pandemic guidelines and access to the health-care system. When COVID numbers began to rise this past January, Dr. Kozoriz enlisted the help of a number of Island Health staff, including Dr. Maki Ikemura, Medical Director, and Emma James, Area Director, Cowichan Region to create a virtual COVID ward based on the previous model with a few adjustments.
“Kelsey has added so much value in that she already had the process and the structure mapped out – she just needed help to bring it to life,” says Dr. Ikemura. “She laid out the process, made the connections with the operations side, looped in the stakeholders, and ensured all the necessary linkages were made. She had assistance, but it really was her tenacity and vision that has made this service possible.”
Dr. Kozoriz has only been in the Cowichan Valley for three years, but her experience as a family physician and background in epidemiology have dovetailed nicely with her COVID work.
“Now that I have journeyed through COVID with so many people, I feel as though I have a good knowledge base about this illness,” she says. “Hopefully moving forward we can leverage this knowledge when we are looking at treatments for long COVID and as it becomes an ongoing respiratory illness within our communities. It’s been an enriching experience.”
Cowichan/South Island media inquiries:
Andrew Leyne
250-370-8908
andrew.leyne@islandhealth.ca